
Dr. Thomas Dudney
Visualization and communication are essential to obtaining successful results when treating anterior aesthetic and complex restorative cases. Visualization is the ability of the clinician to see or picture in their mind the end result before beginning treatment. It sounds easy and for some it may be innate or come naturally, but for others it must be learned or the ability developed. Communication involves both the patient and the dental laboratory. Communication with the patient in these types of cases is obviously critical to success, but it is equally important for the doctor to communicate the necessary information to the laboratory. Well designed and fabricated provisional restorations are the best way to communicate with both the patient and the laboratory. For the patient, the provisionals provide them the ability to ‘preview’ the end result and to evaluate things such as color, size, shape and arrangement of teeth. For the laboratory, the provisionals, once accepted by the patient, provide a blueprint for the fabrication of the definitive restorations including important elements such as length of centrals, tooth proportion, gingival symmetry, smile arc, and buccal corridors. It has been the author’s experience over the years that one of the best ways to improve visualization and communication skills is by attending live patient hands-on courses like the ones taught at the Pacific Aesthetic Continuum (PAC). The following case will describe the treatment of an unusual complex full mouth restoration where visualization of the end result and communication with the lab and patient was critical to success.
The patient presented for a consultation to determine her treatment options. She came in the office wearing an appliance she said had been made for her about 20 years ago. She further stated that she wore her appliance 24 hours a day and could not leave it out for any length of time without experiencing discomfort; therefore, she would only take it out to eat quickly and brush her teeth.
A clinical exam and radiographs revealed recurrent decay around the margins of all of her PFM restorations, gingival inflammation but adequate bone support, and several missing teeth (fig. 1-3). The muscles of mastication were tender to palpation when the appliance was left out for a while, but her joints could be loaded without any pain or soreness. Since
the patient had recurrent decay around all of the existing crowns it was determined that full mouth restorations would be necessary, but the concern was what to do about her dependence on the bite appliance she had been wearing for so long.
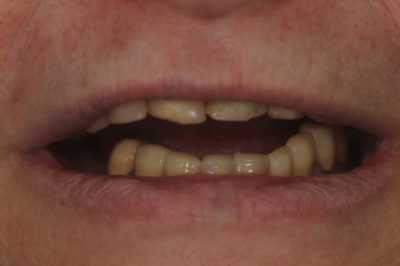
Figure 1
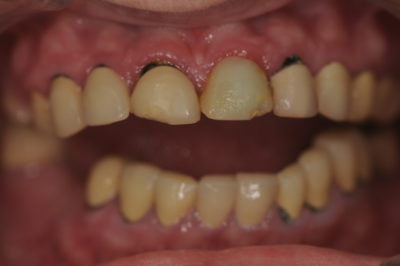
Figure 2
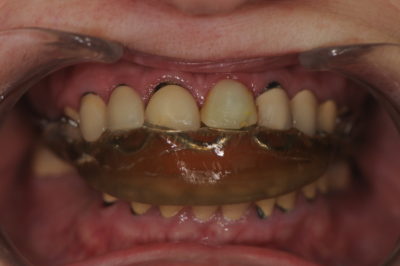
Figure 3
Because the patient was comfortable at the vertical dimension (VD) established by the appliance and her joints were stable, it was reasoned that if she could be restored to the existing VD, but without the appliance in place, she might still be free from discomfort. Therefore, the first goal of the treatment was to try to determine if full mouth restorations were fabricated at the existing VD established by wearing the appliance, would they be acceptable aesthetically. To begin, an interocclusal distance of 22 mm was determined by measuring from the gingival margin of tooth #9 to the gingival margin of tooth #24 with the patient wearing the appliance. After removing the appliance the central incisors (#’s 8 and 9) were mocked up with a flowable composite right over the PFM crowns until 3 mm of material was visible with the patient’s lip at rest (fig. 4). The mock-up also established the length of centrals to be 13mm. Although this incisal edge position and length of centrals was arbitrary and would need to be confirmed with the provisionals, it provided a good starting point for a diagnostic work up.
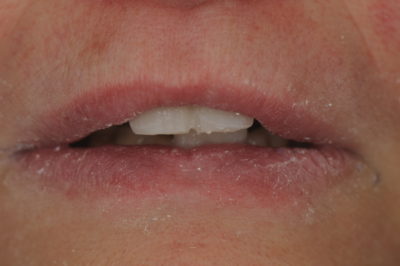
Figure 4
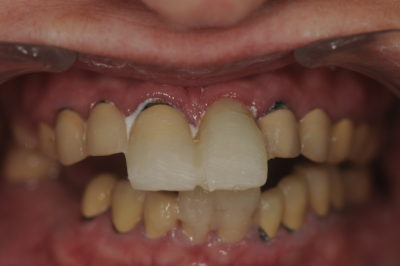
Figure 5
Next, flowable composite was added to the incisal edges of the mandibular centrals (#’s 24 and 25) until an interocclusal distance of 22 mm was obtained when the patient closed together (fig. 5). In addition to the maxillary and mandibular incisal edge position, the length of the central incisors, and the interocclusal distance of 22 mm, the following information was sent to the Pacific Aesthetic Laboratory Group: a series of pre-op photographs, PVS impressions for the study models, a CR bite record, a face bow transfer, a picture and impression of the mock up and a written laboratory prescription requesting a diagnostic wax-up, putty matrices of the wax-up for fabricating provisionals and a PVS CR bite wafer to be relined at the preparation appointment. Also a call was made to Gary Vaughn at the laboratory to discuss what was to be attempted with the case and accomplished with the wax-up.
At the preparation appointment, all of the old crowns were removed, the recurrent decay excavated, the teeth built up and reprepped, and final impressions were taken. The preparation sequence was to prep the maxillary and mandibular posterior teeth on the left side and then reline the PVS CR bite wafer followed by the posterior right side, reline the wafer, and finally the anterior teeth to complete the preparations and then relining the wafer to complete the CR bite record and to maintain the vertical dimension established by the diagnostic wax-up. Additionally a face bow transfer, stick bite, and pictures of the prep shades were taken. All of this information, as well as pictures and impressions of the provisionals and a detailed written prescription, was sent to the laboratory.
Due to the concern for the patient being without the appliance for the first time in many years, she returned the next morning for a post-op evaluation (fig. 6-7). At that time, she stated that her bite felt pretty good and she had not experienced any discomfort. The patient was able to perform phonetic exercises without difficulty speaking and was happy with the size, shape, and color of her teeth and the overall appearance of her smile. Therefore, it was determined that if the patient continued to be comfortable and function properly over the next few weeks, the provisionals would provide an excellent guide for the laboratory to follow and a blueprint for the final restorations functionally, phonetically and aesthetically.
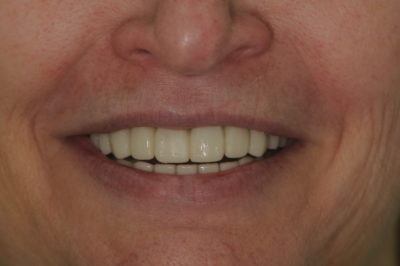
Figure 6
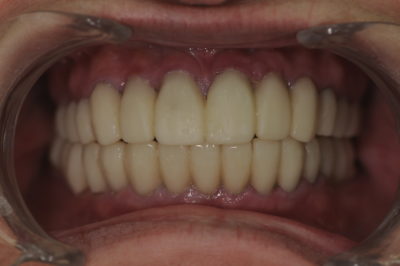
Figure 7
After four weeks, the patient continued to experience no discomfort and returned for the seat appointment. The provisionals in the maxillary arch were removed and the restorations tried in to check fit and contacts. The layered zirconia bridges were seated with a self-adhesive resin cement and the lithium disilicate emax press restorations were bonded with a universal adhesive and dual cure resin cement. After clean up the mandibular arch was seated in the same manner, some minor occlusal adjustments made and the restorations polished. With the patient closed a measurement was taken from the gingival margin of tooth #9 to the gingival margin of tooth #24 and confirmed to be 22 mm, which was the same interocclusal distance when measured originally with the appliance in and maintained with the mock-up, the diagnostic wax-up, and the provisionals. Again, the patient returned for a post-op check appointment at which time she stated that she had continued to experience no discomfort, was happy with her appearance, and most importantly extremely pleased that she no longer had to wear an appliance 24 hours a day (fig. 8-9).
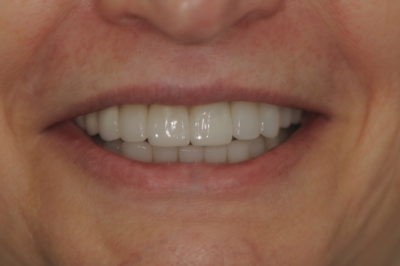
Figure 8
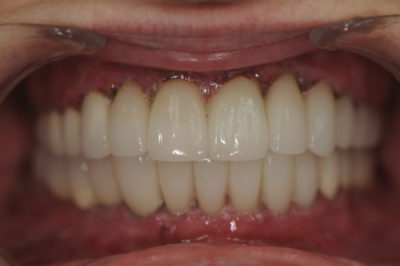
Figure 9
Since this was an unusual case it served as an excellent example of the value of visualization and communication. Visualization of the end result and communicating properly with the patient and the laboratory is obviously critical to success, but is also important in these types of cases to work with a dental laboratory that can provide life-like aesthetic restorations that fit well and require little or no adjustments. If you have questions about my article or if you would like to send a case, please contact the Pacific Aesthetic Laboratory Group at www.pacificaestheticdentalstudio.com, Gary Vaughn, CDT, CTO (916) 786-6740, or via e mail [email protected].
